1 min read
Critical Relay Times and the Future of Stroke and Trauma Treatment
Today is our third and final post in deference to Stroke and Trauma Awareness Month:

Remote radiologist jobs with flexible schedules, equitable pay, and the most advanced reading platform. Discover teleradiology at vRad.

Radiologist well-being matters. Explore how vRad takes action to prevent burnout with expert-led, confidential support through our partnership with VITAL WorkLife. Helping radiologists thrive.

Visit the vRad Blog for radiologist experiences at vRad, career resources, and more.

vRad provides radiology residents and fellows free radiology education resources for ABR boards, noon lectures, and CME.

Teleradiology services leader since 2001. See how vRad AI is helping deliver faster, higher-quality care for 50,000+ critical patients each year.

Subspecialist care for the women in your community. 48-hour screenings. 1-hour diagnostics. Comprehensive compliance and inspection support.

vRad’s stroke protocol auto-assigns stroke cases to the top of all available radiologists’ worklists, with requirements to be read next.

vRad’s unique teleradiology workflow for trauma studies delivers consistently fast turnaround times—even during periods of high volume.

vRad’s Operations Center is the central hub that ensures imaging studies and communications are handled efficiently and swiftly.

vRad is delivering faster radiology turnaround times for 40,000+ critical patients annually, using four unique strategies, including AI.
.jpg?width=1024&height=576&name=vRad-High-Quality-Patient-Care-1024x576%20(1).jpg)
vRad is developing and using AI to improve radiology quality assurance and reduce medical malpractice risk.

Now you can power your practice with the same fully integrated technology and support ecosystem we use. The vRad Platform.

Since developing and launching our first model in 2015, vRad has been at the forefront of AI in radiology.

Since 2010, vRad Radiology Education has provided high-quality radiology CME. Open to all radiologists, these 15-minute online modules are a convenient way to stay up to date on practical radiology topics.

Join vRad’s annual spring CME conference featuring top speakers and practical radiology topics.

vRad provides radiology residents and fellows free radiology education resources for ABR boards, noon lectures, and CME.

Academically oriented radiologists love practicing at vRad too. Check out the research published by vRad radiologists and team members.

Learn how vRad revolutionized radiology and has been at the forefront of innovation since 2001.

%20(2).jpg?width=1008&height=755&name=Copy%20of%20Mega%20Nav%20Images%202025%20(1008%20x%20755%20px)%20(2).jpg)

Visit the vRad blog for radiologist experiences at vRad, career resources, and more.


Explore our practice’s reading platform, breast imaging program, AI, and more. Plus, hear from vRad radiologists about what it’s like to practice at vRad.

Ready to be part of something meaningful? Explore team member careers at vRad.

As I mentioned in my last post, May is both Trauma and Stroke Awareness month. vRad serves hundreds of trauma and stroke centers across the U.S. The intention of this blog series is to provide a behind-the-scenes look into our process for triaging stroke and trauma studies and relaying critical findings.
This is the second in the 3 post series:
Today, let’s talk about Trauma Patients.
Established in 1988 by President Ronald Reagan, May is National Trauma Awareness month; this May is the 29th anniversary of the nationwide StopTheBleed campaign, which works to educate and empower individuals to act in an emergency situation to StopTheBleed – and help protect lives before first responders arrive.
For our part, vRad is proud to provide emergency radiology services to hospitals across the county—in fact, we provide service to approximately 30 percent of hospitals in the United States. Similar to stroke exams, when a trauma occurs, there’s a good chance a vRad radiologist is reading those studies – especially during the night or wee hours of the morning.
We are ALL patients at some point, but many of us have the luxury of knowing “when” our next appointment is. The same is not true for trauma patients whom, by definition, experience an acute injury.
Trauma patients experience an acute traumatic, and many times life-threatening, event that requires immediate medical attention.
The majority of trauma patients have experienced a recent Motor Vehicle Accident (MVA), Gun Shot Wound (GSW), Fall (down steps or in-home injury) or general accidents involving tools or machinery.
Frequently, a trauma patient is entering the hospital after a 911-call or an accident in which the patient was found unresponsive. This can result in patient names such as “Trauma, John”, “Trauma, Female” or other generic patient description. This is a way for the hospital to quickly flag both the underlying urgency and the fact that they are unable to gain basic information from the patient due to their current status.
Given the challenge of communication or uncertainty regarding the extent of the patient’s injuries, trauma patients commonly receive multi-study imaging (Head-to-Toe if necessary). Directly following this imaging, rapid diagnostic interpretations are critical so life-saving measures can be taken.
In early 2014, with the help of our medical leadership team we evaluated our Trauma workflow and identified a few key areas to focus on:
I’d like to elaborate a bit more on our Save-and-Hold feature. We leverage an automated “Save-and-Hold” feature that proactively “Holds” all imaging for a single patient to the original reading radiologist. This helps to create a continuity of care in the event our radiologist needs to call multiple findings to the referring physician, requests follow-up imaging to be performed or the patient has an extensive record of prior exams to review.
Proactively holding exams for a single patient for the same vRad radiologist helps to create a consistent experience and can save everyone time (including the patient) and most importantly, results in better patient care.
This is a critical feature in how we deliver patient care for all non-trauma patients, but it was presenting a unique challenge as it related to our Trauma studies where every minute can make a difference.
Based on this evaluation and discussion with internal and external medical staff, we developed our Trauma Protocol study urgency which enables our clients to designate trauma cases with distinct prioritization and turnaround times.
New Urgency & Prioritization [1 & 2]:
Updating Save-and-Hold [3] Status: The Trauma Protocol urgency bypasses our Save and Hold process and triggers our study unbundling workflow.
If: Urgency = “Trauma”
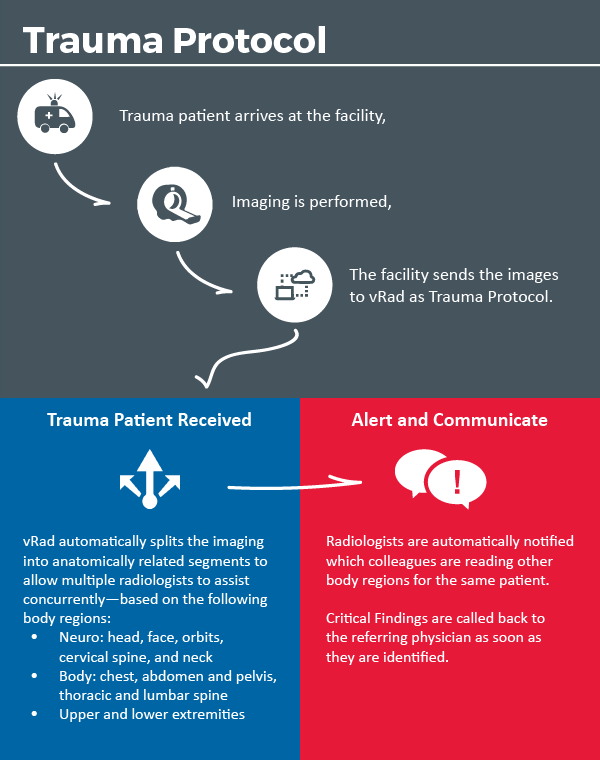
As a result of the changes we made to our Trauma workflow, we have improved our average Trauma study turnaround times by 40 percent (turnaround time statistic compares cases designated as trauma protocol following launch of the vRad Trauma Protocol to comparable cases for the 12-month period prior to launch).
I hope you found this look into our Trauma protocols insightful. Later this month we’ll discuss the future of stroke and trauma care and critical relay times.
Joe Schmugge

1 min read
Today is our third and final post in deference to Stroke and Trauma Awareness Month:

1 min read
May is both Stoke and Trauma awareness month. In recognition of this, we will be publishing a series of 3 posts covering: Stroke information and our...
.png)
1 min read
For the latest information on vRad’s Artificial Intelligence program please visit vrad.com/radiology-services/radiology-ai/ Originally...
vRad (Virtual Radiologic) is a national radiology practice combining clinical excellence with cutting-edge technology development. Each year, we bring exceptional radiology care to millions of patients and empower healthcare providers with technology-driven solutions.
Non-Clinical Inquiries (Total Free):
800.737.0610
Outside U.S.:
011.1.952.595.1111
3600 Minnesota Drive, Suite 800
Edina, MN 55435