1 min read
8 Must-Know CV Tips for Radiologists—Whether Job Hunting or Not
If your Curriculum Vitae isn’t all it could be, you may as well be stacking trophies in a cave. I say this as a longtime radiologist recruiter who...

Remote radiologist jobs with flexible schedules, equitable pay, and the most advanced reading platform. Discover teleradiology at vRad.

Radiologist well-being matters. Explore how vRad takes action to prevent burnout with expert-led, confidential support through our partnership with VITAL WorkLife. Helping radiologists thrive.

Visit the vRad Blog for radiologist experiences at vRad, career resources, and more.

vRad provides radiology residents and fellows free radiology education resources for ABR boards, noon lectures, and CME.

Teleradiology services leader since 2001. See how vRad AI is helping deliver faster, higher-quality care for 50,000+ critical patients each year.

Subspecialist care for the women in your community. 48-hour screenings. 1-hour diagnostics. Comprehensive compliance and inspection support.

vRad’s stroke protocol auto-assigns stroke cases to the top of all available radiologists’ worklists, with requirements to be read next.

vRad’s unique teleradiology workflow for trauma studies delivers consistently fast turnaround times—even during periods of high volume.

vRad’s Operations Center is the central hub that ensures imaging studies and communications are handled efficiently and swiftly.

vRad is delivering faster radiology turnaround times for 40,000+ critical patients annually, using four unique strategies, including AI.
.jpg?width=1024&height=576&name=vRad-High-Quality-Patient-Care-1024x576%20(1).jpg)
vRad is developing and using AI to improve radiology quality assurance and reduce medical malpractice risk.

Now you can power your practice with the same fully integrated technology and support ecosystem we use. The vRad Platform.

Since developing and launching our first model in 2015, vRad has been at the forefront of AI in radiology.

Since 2010, vRad Radiology Education has provided high-quality radiology CME. Open to all radiologists, these 15-minute online modules are a convenient way to stay up to date on practical radiology topics.

Join vRad’s annual spring CME conference featuring top speakers and practical radiology topics.

vRad provides radiology residents and fellows free radiology education resources for ABR boards, noon lectures, and CME.

Academically oriented radiologists love practicing at vRad too. Check out the research published by vRad radiologists and team members.

Learn how vRad revolutionized radiology and has been at the forefront of innovation since 2001.

%20(2).jpg?width=1008&height=755&name=Copy%20of%20Mega%20Nav%20Images%202025%20(1008%20x%20755%20px)%20(2).jpg)

Visit the vRad blog for radiologist experiences at vRad, career resources, and more.


Explore our practice’s reading platform, breast imaging program, AI, and more. Plus, hear from vRad radiologists about what it’s like to practice at vRad.

Ready to be part of something meaningful? Explore team member careers at vRad.

One hard lesson learned during the pandemic is that healthcare providers must be agile—ready to respond quickly and decisively when inevitable crises strike. When it comes to managing radiology staff in particular, some unique challenges and opportunities surfaced in the wake of COVID-19.
As of late 2019, a continued, resurgent demand for radiologists was expected through 2025. Merritt Hawkins projected growth for radiology services, based on an aging population and a strong economy allowing more elective surgeries. They also predicted that the number of radiologists reaching retirement age combined with fewer in residency would constrict the supply of available radiologists to meet the growing demand. (Source: Merritt Hawkins, 2019 Review of Physician and Advanced Practitioner Recruiting Incentives.)
Then in March the reality of COVID-19 hit hard. Imaging demand dropped sharply—in some cases as much as 80%.
By October 2020, radiology administrators and managers responding to the Medical Imaging Confidence Index survey noted that imaging volumes had largely bounced back but that many patients are still reluctant to return to hospitals and imaging centers. "COVID has brought severe uncertainty regarding cash flow and capital allocations. 2021 will bring a new direction and new strategy for growth." (Source: MarkeTech Group, in Auntminnie.com, Oct 16, 2020)
Going forward, practices are wise to include contingencies in their plans that allow them to respond effectively when the next crisis hits. This requires changing how operational costs and business risks are managed, including the hiring and management of the radiologist team.
Successful medical practices will introduce a greater balance of variable costs into business plans, providing needed flexibility for responding to volume changes, making it easier to seize upside opportunities while reducing the potential pain of a decline in demand.
The future of private radiology practices will be impacted by the pandemic in that practices are likely to restructure operational policies and business risks to account for potential sudden volume decreases, as were experienced during the pandemic.
RSNA COVID-19 Task Force, July 2020The Short- and Long-Term Financial Impact of the COVID-19 Pandemic on Private Radiology Practices.

Telemedicine grew at a notable 20% annual rate through the 20-teens, as healthcare providers sought to improve efficiency of care delivery, and patients embraced the convenience of online access to care. In 2020, the coronavirus massively accelerated the use of telehealth. The CDC reported a 154% jump in telehealth visits during the last week of March 2020 vs. the same week in 2019.
In October, the COVID-19 Healthcare Coalition released survey results from the summer, when the group worked with the American Medical Association, state medical societies and other organizations to survey close to 1,600 doctors and other clinicians. Among the project’s key findings:
Hospital administrators rethink infection control
The increased use of remote connections is not limited to interactions between patients and caregivers. In the interest of ensuring a safe workplace for all hospital staff while minimizing patient risk, COVID-19 has forced hospital administrators to rethink infection control, and accelerate telemedicine action plans. For management, that means establishing processes that reduce unnecessary physical contact between physicians, administrators and staff, as well as patients.
This may include policies such as establishing remote workstations where radiologists can effectively conduct diagnostic studies and communicate with ordering physicians, distanced from the physical space occupied by patients and essential care personnel. Reducing the number of people on site at facilities reduces the risk of exposure to coronavirus – or whatever comes next.
Radiologists seek personal safety and burnout relief
As one of the first medical specialties to utilize telemedicine, radiologists are very familiar with the practice of reading remotely and immediately recognized the opportunity to reduce their own COVID-19 exposure risk. In April of 2020, just a few weeks after a national state of emergency was declared in the U.S., teleradiologist job inquires at vRad jumped over 2.5 times the prior 6-month average and remained near those levels through the summer.
.png)
Those responsible for hiring and retaining radiologists will need to take this fundamental shift into consideration as they align the benefits of working for their practice or hospitals with the expectations of radiologists in the post-COVID era.
In the coming years imaging study demand will grow faster than educational institutions will produce new radiologists to help shoulder the load. Simply put, each radiologist faces an expanding caseload.
The aging U.S. population will contribute to increasing consumption of healthcare resources, including medical imaging. Evidence-based medicine is becoming more entrenched, fueling demand for cross-sectional MRI and CT imaging. The rapid development of interventional therapies for chronic illnesses is also adding to the demand for radiologists.
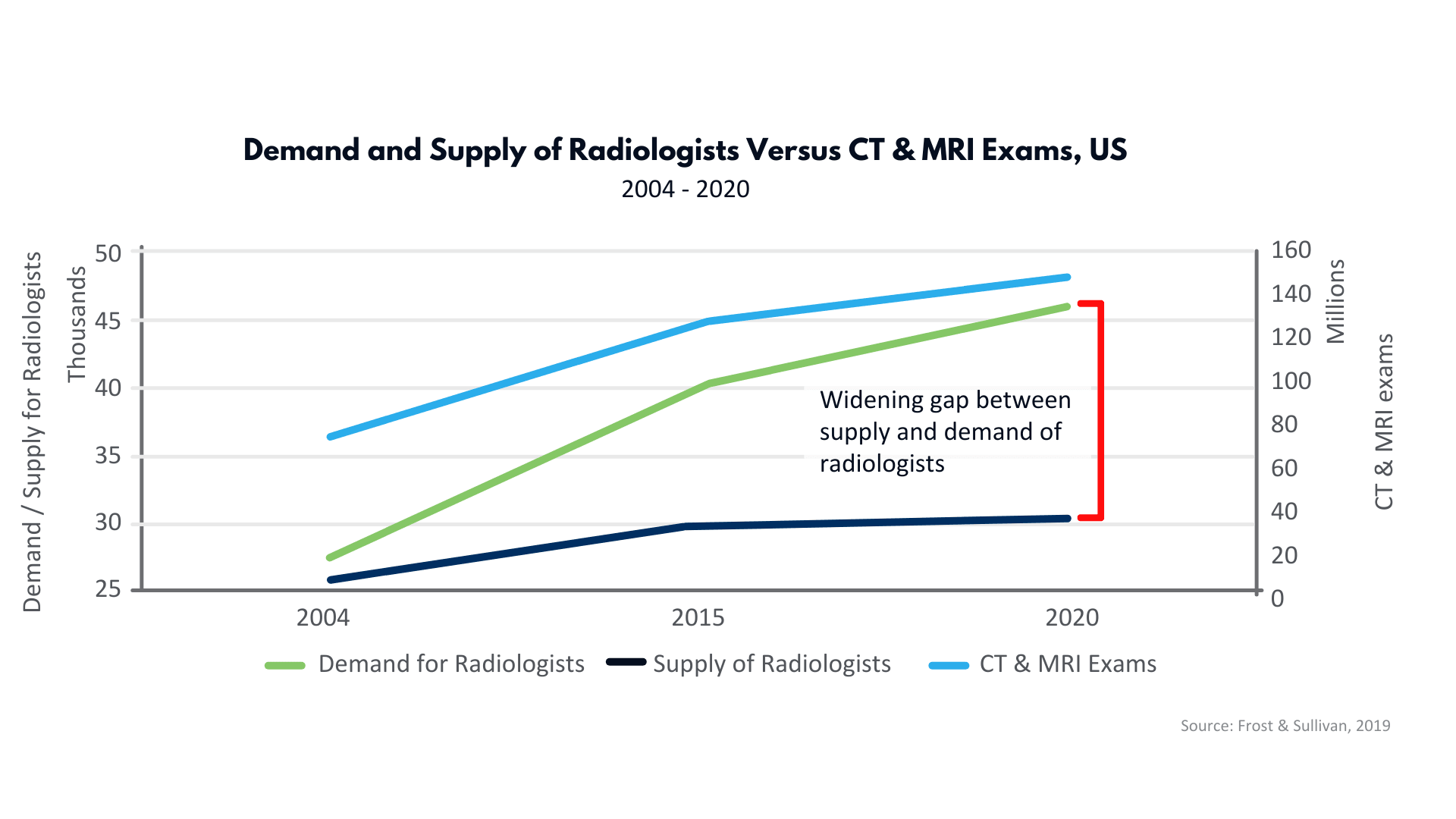 Unfortunately, the number of available radiologists has stagnated in recent years, and projections indicate nominal improvement, or potential worsening, in the future.
Unfortunately, the number of available radiologists has stagnated in recent years, and projections indicate nominal improvement, or potential worsening, in the future.
In addition to fewer people pursuing the profession in medical school, the population of radiologists is aging along with the general population. Of 20,970 in active patient care, 82% of radiologists are age 45 and over, while 53% are age 55 and over.
.png)
A limited supply of radiologists means individual candidates can be more selective about how they choose to practice—in a traditional setting, an academic group, as locum tenens, or with a teleradiology group—and where they choose to practice. Healthcare providers competing for talent from a limited pool will need to differentiate themselves. Each organization must seek to understand what motivates radiologists–including factors beyond compensation like burnout–and demonstrate how they’ve addressed common concerns and created an environment where the candidates can thrive within their unique practice.
For additional hiring best practices, check out this blog from vRad Physician Recruiter, Adam Jones, 7 interview questions for effective radiologist recruiting and hiring.
Back to Blog

1 min read
If your Curriculum Vitae isn’t all it could be, you may as well be stacking trophies in a cave. I say this as a longtime radiologist recruiter who...

1 min read
For the latest information on vRad’s Artificial Intelligence program please visit vrad.com/radiology-services/radiology-ai/ Early hype implied that...
.png)
1 min read
Part-time, locum tenens, moonlighting—in its many forms, practicing radiology on the side is a time-honored tradition. It offers an alternate pathway...
vRad (Virtual Radiologic) is a national radiology practice combining clinical excellence with cutting-edge technology development. Each year, we bring exceptional radiology care to millions of patients and empower healthcare providers with technology-driven solutions.
Non-Clinical Inquiries (Total Free):
800.737.0610
Outside U.S.:
011.1.952.595.1111
3600 Minnesota Drive, Suite 800
Edina, MN 55435